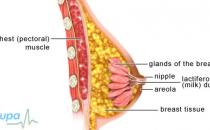
Breast lump removal (lumpectomy)
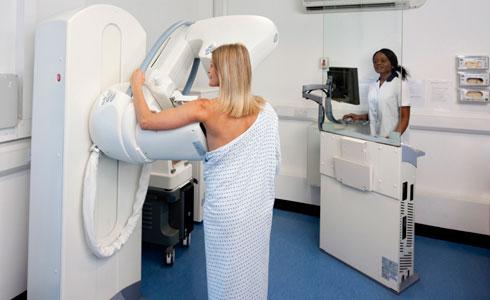
This factsheet is for people who are having a breast lump removed, or who would like information about it.
There are several different types of breast lump. Most of them aren’t cancerous. Breast lump removal (lumpectomy) may be recommended if a lump is cancerous or if it's causing severe discomfort.
You will meet the surgeon carrying out your procedure to discuss your care. It may differ from what is described here as it will be designed to meet your individual needs.
About breast lumps
What are the alternatives?
Preparing for a breast lump removal
What happens during a breast lump removal
What to expect afterwards
Recovering from a breast lump removal
What are the risks?
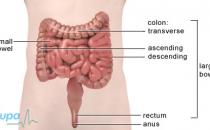
About breast lumps
Breast lumps are very common and most (at least nine out of 10) are benign and not cancerous. Many women will experience one or more breast lumps at some time in their lives. Most benign lumps are:
- cysts – a sac filled with fluid – these are usually drained in the clinic and rarely need to be removed
- fibroadenomas – fibrous and glandular tissue
- breast changes caused by hormones – for example, before a period.
Breast lumps can occur in men too, although they are far less common.
What are the alternatives?
If you have a benign lump, you may have vacuum-assisted core biopsy (VACB) to remove the lump.
If you have a cancerous lump, your treatment will depend on a number of factors, such as whether or not you have been through the menopause, what type of cancer you have and how advanced it is, and whether your cancer has spread. If your lump is large or has spread, you may need to have your whole breast removed (mastectomy) or part of your breast removed (quadrantectomy).
Preparing for a breast lump removal
Your surgeon will explain how to prepare for your operation. For example, if you smoke, you may be asked to stop because smoking increases your risk of getting a chest or wound infection, which can slow your recovery.
Lumpectomy is usually done under general anaesthesia. This means you will be asleep during the operation. You may have the operation and go home the same day, or you may need to stay in hospital for a few days.
Sometimes breast lumps are removed under local anaesthesia. The injection of anaesthetic completely blocks feeling in the area around your breast lump and you will stay awake during the operation. You may be given a sedative with a local anaesthetic. This relieves anxiety and helps you to relax.
If you're having general anaesthesia, you will be asked to follow fasting instructions. This means not eating or drinking, typically for about six hours beforehand. However, it’s important to follow your surgeon’s advice.
Bring in a soft, supportive bra to wear after surgery. Your surgeon or nurse will advise you about the most suitable type of bra.
Your surgeon will discuss with you what will happen before, during and after your procedure, and any pain you might have. This is your opportunity to understand what will happen, and you can help yourself by preparing questions to ask about the risks, benefits and any alternatives to the procedure. This will help you to be informed, so you can give your consent for the procedure to go ahead, which you may be asked to do by signing a consent form.
What happens during a breast lump removal
Your surgeon will make a small cut in your skin over or near the lump, or in an area where the scar won’t be obvious (for example close to your nipple or in the crease under your breast). He or she will cut the lump away along with a section of healthy tissue around it. This is called wide local excision and is done to try and make sure that all the cancerous cells are removed.
Your surgeon will close the cut with fine stitches. He or she will usually place a dressing over the wound. The lump (and healthy tissue) is sent to a laboratory for testing.
If the lump is large, your surgeon may also reconstruct your breast during the operation. This is done by moving muscle into the space the lump has been removed from.
What to expect afterwards
You may need to rest until the effects of the anaesthetic have passed. You may need pain relief to help with any discomfort as the anaesthetic wears off.
Your nurse will give you advice about caring for your healing wound, hygiene and bathing before you go home. You may be given a date for a follow-up appointment.
You will need to arrange for someone to drive you home. Try to have a friend or relative stay with you for the first 24 hours.
The length of time your dissolvable stitches will take to disappear depends on what type you have. However, for this procedure they should usually disappear in about seven to 10 days.
Recovering from a breast lump removal
If you need pain relief, you can take over-the-counter painkillers such as paracetamol or ibuprofen. Always read the patient information leaflet that comes with your medicine and if you have any questions, ask your pharmacist for advice.
General anaesthesia temporarily affects your co-ordination and reasoning skills, so you must not drive, drink alcohol, operate machinery or sign legal documents for 48 hours afterwards. If you're in any doubt about driving, contact your motor insurer so that you're aware of their recommendations, and always follow your surgeon’s advice.
After the operation, your wound may feel sore and you may find it more comfortable not to wear a bra. When the pain improves, you should wear a supportive bra.
Your nurse or physiotherapist may give you some exercises to do to prevent stiffness in your arm and shoulder.
Don't carry or lift anything heavy, or drive, while your wound is healing. This is likely to be for about 2 weeks.
What are the risks?
Breast lump removal is commonly performed and generally safe. However, in order to make an informed decision and give your consent, you need to be aware of the possible side-effects and the risk of complications of this procedure.
Side-effects
These are the unwanted but mostly temporary effects of a successful procedure.
Side-effects of breast lump removal include:
- bruising and some swelling – this should improve as your wound heals
- numbness or pins and needles
- scarring – you will have a scar but this should gradually fade
Complications
This is when problems occur during or after the operation. Most people are not affected. The possible complications of any operation include an unexpected reaction to the anaesthetic, infection, excessive bleeding or developing a blood clot, usually in a vein in the leg (deep vein thrombosis, DVT).
Specific complications of breast lump removal are uncommon, but can include:
- an unevenness in the size and shape of your breast
- a temporary build up of fluid under your wound or in your arm (called a seroma) – this is more likely to happen if you have had breast reconstruction
- the breast lump may come back in the future and need further surgery or treatment
The exact risks are specific to you and differ for every person, so we have not included statistics here. Ask your surgeon to explain how these risks apply
This section contains answers to common questions about this topic. Questions have been suggested by health professionals, website feedback and requests via email.
Will my breast look different after a lumpectomy?
Can breast lumps come back again?
Do I need to have a benign breast lump removed?
Will my breast look different after a lumpectomy?
Your breast may look slightly different after having a breast lump removed (lumpectomy). You will also have a scar from surgery, though this will fade and become less noticeable over time. Your surgeon will do everything possible to make sure any change to your breast shape or scaring is as small as possible.
Explanation
Usually, there are few noticeable changes to your breast after a breast lump removal. Any change in your breast size or shape will be minimal and shouldn’t affect your bra size. Most women don’t need to have breast reconstruction unless the lump is very large.
Talk to your surgeon or nurse about how your breast will look after you have had your surgery. You may also find it helpful to talk to other women who have had a breast lump removed.
You will have a small scar after surgery. This usually fades gradually and becomes less noticeable. However, some people develop unusual red or raised scars (keloids) and these can take longer to improve. Speak to your doctor if you have any concerns.
Further information
-
Breast Cancer Care
0808 800 6000
www.breastcancercare.org.uk -
Macmillan Cancer Support
0808 808 0000 - www.macmillan.org.uk
Sources
- About breast reconstruction. Cancer Research UK. www.cancerhelp.org.uk, published May 2009
- Living with breast cancer surgery. Cancer Research UK. www.cancerhelp.org.uk, published May 2009
Can breast lumps come back again?
Yes, breast lumps can re-occur.
Explanation
Breast lumps can come back again. If you had a cancerous lump removed, then you’re more at risk of developing another tumour compared to a woman who hasn’t had cancer. If breast cancer is going to come back, then it’s most likely to happen in the two years following your surgery. Breast cancer can still come back 10 or 20 years after you’re first diagnosed. However, this is uncommon and, in general, the more time that passes after your diagnosis, the less likely it is that your cancer will come back.
Breast lumps that are cysts often come back and refill with fluid. If this happens, visit your GP to have it checked.
It's important to check your breasts regularly by looking at them and feeling them. Once you know how your breasts usually look and feel, you will notice if anything changes. Talk to your GP or breast surgeon if you spot any changes in your breasts.
Further information
-
Breast Cancer Care
0808 800 6000
www.breastcancercare.org.uk -
Macmillan Cancer Support
0808 808 0000 - www.macmillan.org.uk
Sources
- Breast cancer risk factors. Cancer Research UK. www.cancerresearchuk.org, published January 2010
- Statistics and outlook for breast cancer. Cancer Research UK. www.cancerhelp.org.uk, published May 2009
- Breast cysts. Breast Cancer Care. www.breastcancercare.org.uk, published November 2009
Do I need to have a benign breast lump removed?
No, you don't need to have a benign (non-cancerous) breast lump removed. However, your doctor may suggest surgery if the lump is large, growing in size, or is causing discomfort.
Explanation
Your surgeon will usually only suggest having a breast lump removed if the lump is cancerous. Benign lumps usually get better without treatment.
If the lump is causing you severe pain and discomfort, your surgeon may suggest a lumpectomy (breast lump removal).
When considering surgery, you need to be aware of the possible side-effects and the risk of complications of the procedure. Discuss the risks and benefits with your surgeon and be sure the benefits of surgery outweigh the risks.
Further information
-
Breast Cancer Care
0808 800 6000
www.breastcancercare.org.uk -
Breakthrough Breast Cancer
08080 100 200
www.breakthrough.org.uk
Sources
- Benign breast conditions. Breast Cancer Care. www.breastcancercare.org.uk, published November 2009
Related topics
- Breast awareness and screening
- Breast cancer
- Breast lump investigation
- Breast lump removal (lumpectomy)
- Caring for surgical wounds
Related topics
Further information
-
Breast Cancer Care
0808 800 6000
www.breastcancercare.org.uk -
Macmillan Cancer Support
0808 808 0000 - www.macmillan.org.uk
Sources
- Breast cancer symptoms. Cancer Research UK. www.cancerhelp.org.uk, published April 2009
- Dixon MJ, Leonard RCF, editors. Understanding breast disorders. Poole, Dorset:] Family Doctor Publications in association with the British Medical Association, 2002
- Fibroadenoma. Breast Cancer Care. www.breastcancercare.org.uk, published November 2009
- Which treatment for breast cancer? Cancer Research UK. www.cancerhelp.org.uk, accessed 21 March 2010
- Types of breast cancer surgery. Cancer Research UK. www.cancerhelp.org.uk, accessed 21 March 2010
- After your breast cancer operation. Cancer Research UK. www.cancerhelp.org.uk, published May 2009
- Lumpectomy and immediate breast reconstruction. Macmillan Cancer Support. www.macmillan.org.uk, published November 2008
- Having your breast cancer operation. Cancer Research UK. www.cancerhelp.org.uk, published May 2009
- After surgery for breast cancer. Macmillan Cancer Support. www.macmillan.org.uk, published September 2008
- After surgery. Breast Cancer Care. www.breastcancercare.org.uk, published December 2009