Coronary artery bypass graft (CABG) surgery
This factsheet is for people who are having a coronary artery bypass graft (CABG), or who would like information about it.
CABG is surgery to treat coronary heart disease. A blood vessel is taken from the chest, leg or arm and used to bypass a narrowed or blocked coronary artery.
You will meet the surgeon carrying out your procedure to discuss your care. It may differ from what is described here as it will be designed to meet your individual needs.
How coronary artery bypass graft is carried out
About CABG
What are the alternatives to CABG?
Preparing for your CABG
About the operation
What to expect afterwards
Recovering from CABG
What are the risks?
How coronary artery bypass graft is carried out
The information on the video provided does not constitute advice on diagnosis or the treatment for heart disease and such advice should always be sought from a doctor or another suitably qualified health professional.
About CABG
The coronary arteries are blood vessels that supply your heart with oxygen and nutrients. If you have coronary heart disease, they are narrowed or blocked. This can starve your heart of oxygen, which causes angina (the feeling of chest pain, chest tightness and breathlessness). The pain or discomfort sometimes spreads to other parts of the body, for example, the arms.
CABG surgery aims to bypass the blocked arteries to increase the blood flow to the heart muscle. A new blood vessel (a graft) is attached from your aorta (the main artery leaving your heart) to a point in the coronary artery beyond the blockage. Your graft(s) can be created from blood vessels (arteries or veins) taken from your chest wall, leg or arm.
CABG won’t cure coronary heart disease so it’s possible that blockages may re-occur either in the grafts or in other coronary arteries. The operation helps to manage your symptoms. You will need to make lifestyle changes to help prevent your condition from getting worse.
What are the alternatives to CABG?
There are several alternative treatments available. Some examples are listed below.
- Medicines, such as calcium channel blockers, beta-blockers, statins and anti-platelets may improve your symptoms or prevent your condition from getting worse.
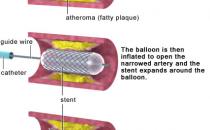
- Coronary angioplasty – a plastic tube called a catheter is inserted into a blood vessel (either in your groin or your wrist) and used to open up the narrowed arteries so that blood flows more easily to the heart muscle. A stent (a small metal tube) may be used to help keep the artery open.
Your treatment will depend on the condition of your coronary arteries. Your surgeon will advise you which treatment is most suitable for you.
Preparing for your CABG
Your surgeon will explain how to prepare for your operation. For example, if you smoke you will be asked to stop, as smoking increases your risk of getting a chest and wound infection, which can slow your recovery.
You will spend about a week in hospital. The operation is usually done under general anaesthesia. This means you will be asleep during the operation.
You will be asked to follow fasting instructions. This means not eating or drinking, typically for about six hours beforehand. However, it’s important to follow your surgeon’s advice.
Your surgeon will discuss with you what will happen before, during and after your procedure, and any pain you might have. This is your opportunity to understand what will happen, and you can help yourself by preparing questions to ask about the risks, benefits and any alternatives to the procedure. This will help you to be informed, so you can give your consent for the procedure to go ahead, which you may be asked to do by signing a consent form.
You may be asked to wear compression stockings to help prevent blood clots forming in the veins in your legs. You may need to have an injection of an anticlotting medicine called heparin as well as, or instead of, wearing compression stockings.
About the operation
The procedure may take up to four hours.
Your surgeon will first prepare the graft. To remove a blood vessel from your leg, your surgeon may make a cut along the inside of your leg, between your ankle and groin to reach the vein. Sometimes an artery in your lower arm is used as a graft, and your surgeon will make a cut from your wrist to your elbow to remove the vein.
To reach your heart, your surgeon will make a cut about 25cm (10 inches) long, down the middle of your breastbone (sternum) and open your chest.
Your surgeon may attach the new grafts while your heart is still beating. However, it’s more common to temporarily stop the heart and divert the blood to a heart-lung (bypass) machine. This helps to keep your blood oxygenated and maintains your blood circulation during the operation.
The grafts will be attached and your heart will be restarted. Your breastbone will be rejoined using wires and the skin on your chest will be closed, often, with dissolvable stitches.
Keyhole surgery
CABG can be done using keyhole surgery.
To remove the blood vessel from your leg, your surgeon may make small cuts near your knee and pass special instruments through the cuts to take the vein. Your surgeon will look at a monitor to see inside your leg. This keyhole technique is called endoscopic saphenous vein harvesting.
To reach your heart, your surgeon will make two or three small cuts on your chest and pass special instruments through the cuts to perform the operation. Your surgeon will look at a monitor to see inside your chest.
Keyhole surgery isn’t suitable for everybody – your surgeon will advise you if it’s appropriate for you.
What to expect afterwards
After your operation, you will be taken to the intensive care unit (ICU) and will be closely monitored for about 24 hours before you go back to your ward.
When you wake up you will be connected to machines that record the activity of your heart, lungs and other body systems. These might include a ventilator machine to help you breathe.
You may need pain relief to help with any discomfort as the anaesthetic wears off.
You may have a catheter to drain urine from your bladder into a collection bag. You may also have tubes running out from the wound. These (chest tubes) drain fluid into another bag and are usually removed after a day or two.
You may also be wearing compression stockings on your legs to help maintain circulation. You will be encouraged to get out of bed and move around as this helps prevent chest infections and blood clots in your legs.
A physiotherapist (a health professional who specialises in maintaining and improving movement and mobility) will usually visit you every day to guide you through exercises designed to help your recovery.
When you’re ready to go home, you will need to arrange for someone to drive you home. Try to have a friend or relative stay with you for the first week or two.
Your nurse will give you some advice about caring for your healing wounds before you go home. You may be given a date for a follow-up appointment.
The wires holding your breastbone together are permanent. The length of time your dissolvable stitches will take to disappear depends on what type you have. For this procedure, they should usually dissolve in about six weeks.
Recovering from CABG
If you need pain relief, you can take over-the-counter painkillers such as paracetamol or ibuprofen. Always read the patient information leaflet that comes with your medicine and if you have any questions, ask your pharmacist for advice.
Your breastbone should take about six to eight weeks to heal but it can take up to three months to recover fully. Don’t lift heavy objects or do any strenuous activity until the breastbone has fully healed. Your surgeon will give you advice about how soon you can return to work.
Follow your surgeon’s advice about driving. You shouldn’t drive until you’re confident that you could perform an emergency stop without discomfort. If you drive a lorry or a bus you need to notify the DVLA about your operation and you will be disqualified from driving for three months. You will need to take an exercise test before you are allowed to drive again.
What are the risks?
CABG is commonly performed and generally safe. However, in order to make an informed decision and give your consent, you need to be aware of the possible side-effects and the risk of complications.
Side-effects
These are the unwanted but mostly temporary effects of a successful procedure, for example feeling sick as a result of the general anaesthetic. Side-effects of CABG include:
- soreness, swelling and bruising around your healing wound – this can last up to a month
- scarring – you will have permanent scars, they will be pink and noticeable at first, but usually fade over time
Complications
This is when problems occur during or after the procedure. Most people are not affected. The possible complications of any operation include an unexpected reaction to the anaesthetic, infection, excessive bleeding or developing a blood clot, usually in a vein in the leg (deep vein thrombosis, DVT).
Specific complications of CABG are rare but can include a heart attack, stroke or death – however, it’s important to consider that having no treatment, or an alternative treatment, may have a higher risk.
If you have keyhole surgery, there’s a chance your surgeon may need to convert to open surgery if it’s impossible to complete the operation safely using the keyhole technique.
The exact risks are specific to you and differ for every person, so we have not included statistics here. Ask your surgeon to explain how these risks apply to you.
What can I do to prevent my arteries narrowing?
My doctor says that I may be able to have ‘off-pump’ CABG. What is this?
Since my CABG I have been feeling depressed. Is this normal?
What can I do to prevent my arteries narrowing?
To help prevent your arteries narrowing you can take medicines and make lifestyle changes. That way you may not need surgery to treat coronary heart disease.
Explanation
If you have coronary heart disease, it’s not possible to reverse the damage that has already taken place. If you have angina (the feeling of chest pain, chest tightness and breathlessness), you may be able to manage your symptoms with medicines. Medicines for angina include:
• aspirin
• ivabradine (eg procoralan)
• beta-blockers (eg atenolol, bisoprolol)
• long-acting nitrates (eg isosorbide mononitrate)
• calcium-channel blockers (eg nifedipine)
• potassium-channel activators (eg nicorandil)
• statins (eg simvastatin)
These medicines aren’t suitable for everyone. Your doctor will advise you which is best for you.
Life-style changes can help to prevent your condition from getting worse. These include:
- giving up smoking
- getting medical treatment to reduce your blood pressure and cholesterol levels, if high
- maintaining a healthy weight and eating a balanced diet
- staying active
Your doctor can advise you on how you can make changes to keep your heart healthy.
Further information
British Heart Foundation
0300 330 3311
www.bhf.org.uk
Sources
- Angina. Clinical Knowledge Summaries. www.cks.nhs.uk, accessed 21 June 2010
- Lipid modification – primary and secondary CVD prevention. Clinical Knowledge Summaries. www.cks.nhs.uk, accessed 21 June 2010
- Having heart surgery. British Heart Foundation. www.bhf.org.uk, published July 2010
My doctor says that I may be able to have 'off-pump' CABG. What is this?
‘Off-pump’ CABG (OPCAB) or ‘beating heart surgery’ is an alternative technique to conventional CABG that doesn’t require you to be connected to a heart-lung (bypass) machine.
Explanation
In a conventional CABG operation your heart is stopped using medicines containing potassium. Your heart and lungs are then connected to a bypass machine that takes over to add oxygen to your blood and maintain your circulation.
OPCAB is an alternative technique where the heart continues to beat as the surgeon performs the bypass grafts. OPCAB is thought to be just as effective as a traditional CABG operation but may have a slightly lower risk of complications. However, research is ongoing to determine the safety of OPCAB and whether it is as effective as the traditional technique.
Further information
British Heart Foundation
0300 330 3311
www.bhf.org.uk
Sources
- Debate continues over use of off-pump CABG – eyes on evidence commentary. NHS Evidence. www.evidence.nhs.uk, published February 2010
- Off-pump coronary artery bypass (OPCAB). National Institute for Health and Clinical Excellence (NICE), 2004. Interventional Procedure Guidance 35. www.nice.org.uk
- Shroyer Al, Grover Fl, Hattler B, et al. On-pump versus off-pump coronary-artery bypass surgery. New Engl J Med 2009; 361(19):1827–37
Since my CABG I have been feeling depressed. Is this normal?
Yes. Feeling depressed, unhappy or anxious is often a natural reaction to having major surgery.
Explanation
After your surgery you may find that you feel depressed or unhappy. This is quite common and you may even find that you experience a range of emotions, from being happy that the operation is over to being sad that it will take time to recover.
It’s a good idea to have someone stay with you for the first week or two to keep you company and to take care of you. If you live alone, it should be possible to arrange extra care visits.
When you get out of the hospital you should notify your GP so that he or she can provide you with any care that you may need.
Further information
British Heart Foundation
0300 330 3311
www.bhf.org.uk
Royal College of Psychiatrists
020 7235 2351
www.rcpsych.ac.uk
Sources
- Having heart surgery. British Heart Foundation. www.bhf.org.uk, published July 2010
Related topics
- Depression
- Healthy eating
- Looking after your heart
[Box] Coronary artery bypass graft (CABG) surgery factsheet.
Visit the coronary artery bypass graft (CABG) surgery health factsheet for more information.
Related topics
- Angina
- Caring for surgical wounds
- Compression stockings
- Coronary angioplasty
- Deep vein thrombosis
- Diagnosing heart conditions
- General anaesthesia
- Heart attack
- Over-the-counter painkillers
Further information
British Heart Foundation
0300 330 3311
www.bhf.org.uk
Sources
- CABG information. The Society of Thoracic Surgeons. www.sts.org, accessed 21 June 2010
- Angina. Clinical Knowledge Summaries. www.cks.nhs.uk, accessed 21 June 2010
- Having heart surgery. British Heart Foundation. www.bhf.org.uk, published July 2010
- Coronary bypass surgery. British Heart Foundation. www.bhf.org.uk, accessed 21 June 2010
- Endoscopic saphenous vein harvest for coronary artery bypass grafting. National Institute for Health and Clinical Excellence (NICE), 2010. Interventional procedure guidance 343. www.nice.org.uk
- Interventional procedures overview of totally endoscopic robotically assisted coronary artery bypass surgery. National Institute for Health and Clinical Excellence (NICE), 2005. www.nice.org.uk
- At a glance guide to the current medical standards of fitness to drive. Driver and Vehicle Licensing Agency (DVLA), February 2010. www.dft.gov.uk
- CABG (conventional, MIDCAB or OPCAB) versus PTCA (with or without stenting). BMJ Clinical Evidence. www.clinicalevidence.bmj.com, accessed 21 June 2010
- Biancari F, Tiozzo V. Staples versus sutures for closing leg wounds after vein graft harvesting for coronary artery bypass surgery. Cochrane Database of Systematic Reviews 2010, Issue 5.
doi:10.1002/14651858.CD008057.pub2.